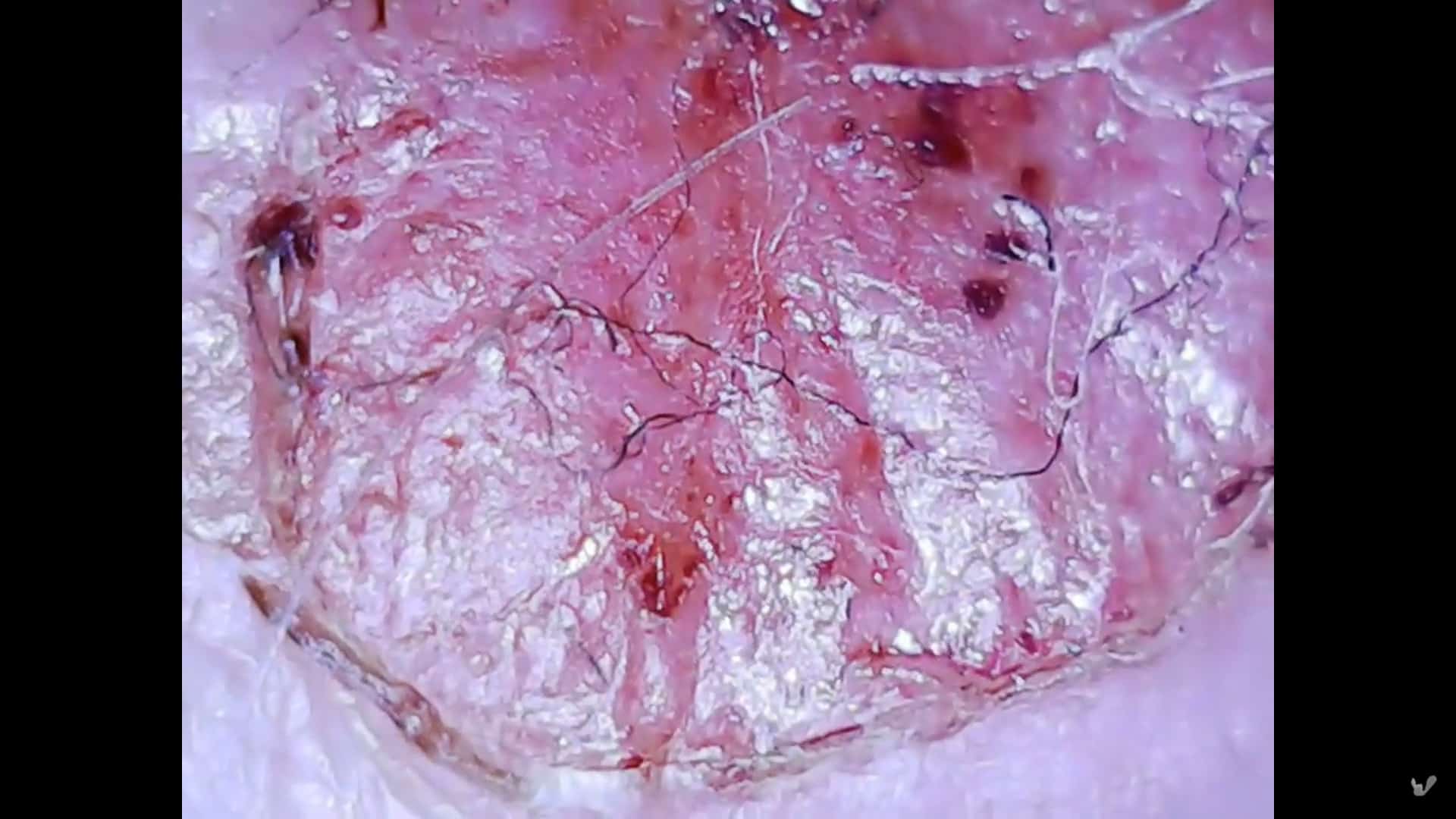
Morgellons disease is a polarized topic in the medical community with two opposing points of view that are incompatible. The prevailing point of view is that MD is a psychiatric disorder with a delusional etiology. The minority emerging point of view is based on recent clinical, molecular and histopathological evidence that challenges the prevailing view and suggests an infectious etiology for Morgellons disease. When challenging a prevailing well-established point of view, new evidence will always be met with opposition, skepticism and sometimes outright hostility.
Evidence supporting the hypothesis that Morgellons disease is an infectious process is published in many reputable, PubMed-indexed medical journals, including but not limited to: the International Journal of General Medicine, Clinical Cosmetic and Investigational Dermatology, BMC Dermatology, F1000 Research, Healthcare (Basel), Dermatology Reports, and Psychosomatics. Stricker, Middelveen and Fessler are not alone in supporting this point of view. They do not work in isolation, but collaborate with other laboratories. The evidence supporting an infectious process includes experiments performed in at least 12 different institutions that include universities, commercial laboratories or clinical practices, located in 4 different countries and include a diverse group of independent individuals.
Resultant peer-reviewed papers, many of which are primary research, have repeatedly demonstrated an association between MD and spirochetal infection (predominantly Borrelia species) that is statistically significant. Evidence includes serological, histopathological and molecular evidence showing Borrelia exposure and/or infection in MD patients. Furthermore, Borrelia species have been cultured and genetically characterized from skin and other clinical specimens taken from Morgellons disease subjects, and culture is the ultimate proof of active infection. To date, Borrelia DNA has been detected in skin specimens taken from Morgellons subjects by at least seven independent laboratories and that fact is available by reading published papers available through a PubMed search. Collaborative studies that included Stricker, Middelveen and/or Fessler as author, in which Borrelia DNA was detected in specimens taken from Morgellons patients, were performed by four independent laboratories (University of New Haven, West Haven, CT; Australian Biologics, Sydney, NSW, Australia, IGeneX Reference Laboratories, Milpitas, CA, and UC -Irvine, Irvine, CA). As indicated in presentations made at Charles E Holman Foundation conferences, two additional laboratories, Mt Allison University in Sackville, NB, Canada, and Oklahoma State University, have also detected Borrelia DNA in MD skin cultures/and or skin specimens.
Showing causation is not straightforward. There is no perfect method for demonstrating disease causation. Various proposed methods for demonstrating causation are not checklists that must be met. However, the more criteria are met, the more likely a causal relationship is to exist. Correlation is the first step in showing causation. Currently there is more than a mere correlation shown between MD and Borrelia. Many of the criteria in Koch’s postulates, the Bradford Hill criteria for causation, and the criteria listed by Fredricks and Relman have been met. [1-3] The evidence that Borrelia infection is associated with MD has never been disproven by the opposition in peer-reviewed literature. If those holding the majority point of view feel that there is sufficient evidence to show an infectious etiology for Morgellons disease is wrong then they should challenge the evidence with published, peer-reviewed rebuttal.
In contrast, a 2018 review paper by Middelveen et al. published in a reputable PubMed-indexed medical journal [4] provides a detailed evaluation of the evidence supporting both points of view, and addresses significant flaws in the papers that support the point of view that MD is a purely delusional disorder. In contrast, the majority who hold the prevailing point of view have failed to identify specific flaws in the data or methods used by Stricker, Middelveen, Fessler, and their other collaborators, but instead have relied on personal attacks and their own preconceived point of view.
At the very least, the emerging body of evidence that concludes an infectious process causes Morgellons disease clearly demonstrates that society is dealing with an unexplored and poorly defined chronic bacterial infection that has affected individuals around the world and needs to be recognized so that steps can be taken to improve quality of life and to lessen if not alleviate the burden of this challenging illness. Attempts to shut down open debate and discussion in medicine stifle medical science. If not for open debate we would still believe in the miasma theory of disease, steadfastly believing that infectious diseases, such as cholera, syphilis, chlamydia, or even the Black Death are noxious forms of “bad air”. Medicine needs to evolve and challenging prevailing thought through open debate is an essential part of that process.
References
- Fedak KM, Bernal A, Capshaw ZA, Gross S. Applying the Bradford Hill criteria in the 21st century: how data integration has changed causal inference in molecular epidemiology. Emerg Themes Epidemiol. 2015;12:14. Published 2015 Sep 30. doi:10.1186/s12982-015-0037-4
- Fredericks DN, Relman DA. Sequence-based identification of microbial pathogens: a reconsideration of Koch’s postulates. Clinical Microbiology Reviews Jan 1996, 9 (1) 18-33; DOI: 10.1128/CMR.9.1.18
- Middelveen MJ, Martinez RM, Fesler MC, Sapi E, Burke J, Shah JS, Nicolaus C, Stricker RB. Classification and Staging of Morgellons Disease: Lessons from Syphilis. Clin Cosmet Investig Dermatol. 2020 Feb 7;13:145-164. doi: 10.2147/CCID.S239840. PMID: 32104041; PMCID: PMC7012249.
- Middelveen MJ, Fesler MC, Stricker RB. History of Morgellons disease: from delusion to definition. Clin Cosmet Investig Dermatol. 2018 Feb 9;11:71-90. doi: 10.2147/CCID.S152343. PMID: 29467580; PMCID: PMC5811176
- Middelveen MJ, Stricker RB. Morgellons disease: a filamentous borrelial dermatitis. Int J Gen Med. 2016 Oct 14;9:349-354. doi: 10.2147/IJGM.S116608. PMID: 27789971; PMCID: PMC5072536.